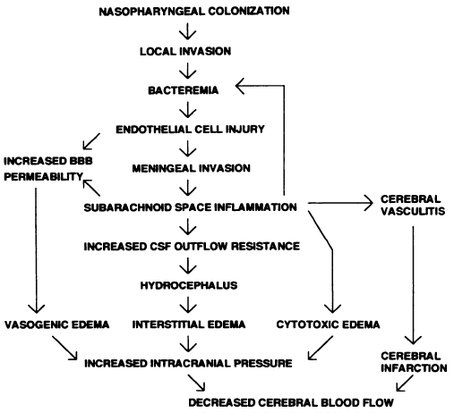
Routes of Infection:
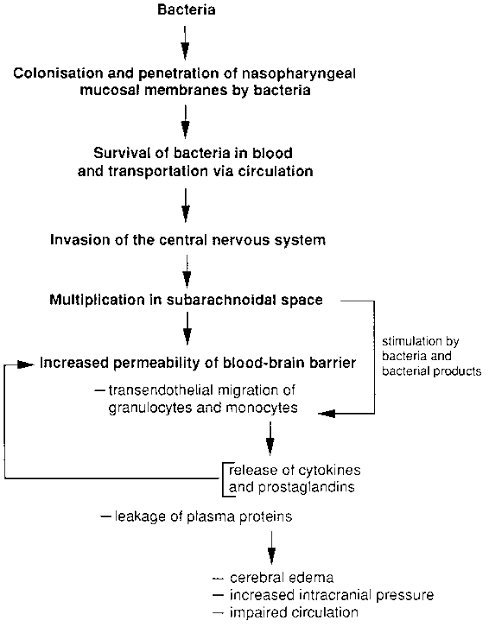
Organisms may gain access to the meninges by several routes
A. Hematogenous spread:
This is the most common routes, where entry into the subarachnoid space is gained through the chotoid plexus or through other blood vessels of the brain.
B. Direct spread from an infected site:
Direct spread from an infected site present close to meninges–Otaitis media, mastoiditis, sinusitis etc.
C. Anatomical defects in Central Nervous system (CNS) :
It may occur as a result of surgery., trauma, congenital defects which can allow organisms for ready and easy access for CNS
D. Direct intraneural spread along the nerve:
This is the least common route, occurs in case of rabies virus or herpex simplex virus infection.
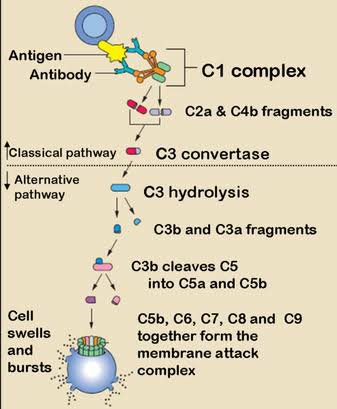
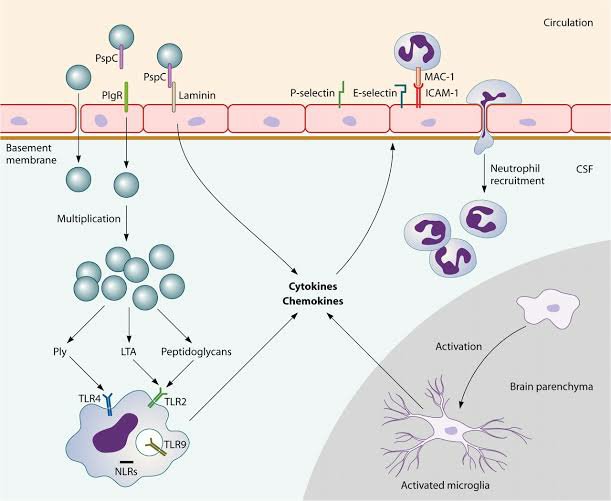
Predisposing factors:
Pathogenesis of meningitis depends upon various host and microbial factors.
A. Age
Neonates have the highest prevalence of meningitis;probably due to,[1] their immature immune system, [2] acquiring the colonised organisms from mother’s birth canal(e.g. Group B streptococcus) [3] permeability of blood brain barrier.
B. Vaccination:
Widespread vaccination is shown to reduce the incidance of meningitis due to the particular agents, e.g. low incidence of H. influenzae meningitis following implementation of Hib vaccination
C. Factors that promote infection at primary site:
Because respiratory tract is the primary portal of entry for many etiological agents of meningitis, the factors that predisposed to respiratory infections can also increase the likelihood of development of meningitis. Such factors including alcoholism, diabetes, immunosuppression, splenectomy, etc.
D. Present of CSF shunts:
Present of CSF shunts can also directly predisposed to the pathogen entry
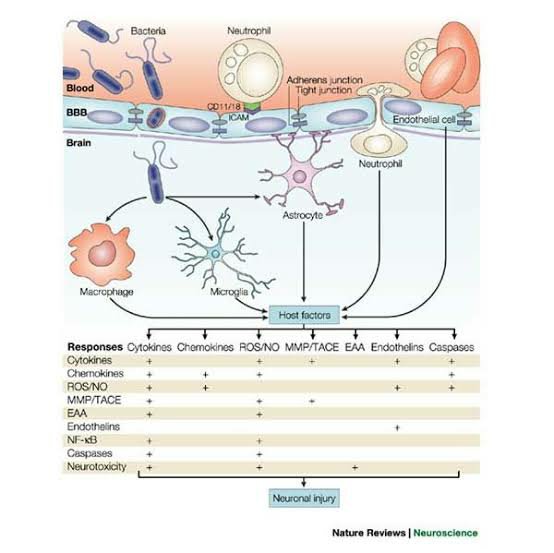
E. Breach in the blood brain barrier (BBB) :
Organisms can gain access through BBB by:
- Loss of capillary integrity by disrupting rhe tight junction of BBBT
- ransport within circulatory phagocytes
- Crossing the endothelial cells by transport within the endothelial cell vacuoles
F. Microbial virulence factors:
It may also contribute to the pathogenesis such as:
- Capsular polysaccharideL
- ipoteichoic acid
- IgA proteases